What are the symptoms of hyperthyroidism?
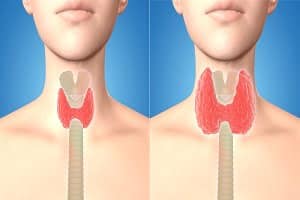
Although thyroid gland is a small gland but the thyroid hormone produced affects each and every cell of the body. Thyroid hormone is an important hormone that plays a significant role in metabolism. Hyperthyroidism may be present with significant symptoms. Since overactive thyroid gland increases the metabolism, many individuals initially have a lot of energy. However, as the body tends to break down, feeling lethargic is quite common. However, not everyone with hyperthyroidism will experience all of the symptoms.

Read about thyroid gland and hyperthyroidism (overactive thyroid).
Increased level of thyroid hormone causes hand tremors, anxiety, sleep depravedness, brittle hair, thinning of the skin, shortness of breath, increased perspiration and muscle weakness particularly in thighs and arms.
Hyperthyroidism may also lead to sudden paralysis.
The person suffering may have frequent bowel movement and diarrhea. Sudden loss of weight even after good appetite is another symptom of overactive thyroid. About 10% of people suffering from hyperthyroidism report weight gain.
In women, hyperthyroidism results in the decrease of menstrual flow and delayed periods. It also increases the length of the menstrual cycle in adolescent girls. At first, these symptoms are mistaken as nervousness and anxiety due to stress.
An excess amount of thyroid hormone is also known to aggravate the effect of the sympathetic nervous system. This speeds up many biological functions and sometimes resembles over dosage of epinephrine. This eventually fastens the heart beat and induces tremors in hands and legs. Moreover, its increased level in blood lowers serum cholesterol.
Apart from weight loss in spite of increased appetite, high blood sugar, excessive urination, and excessive thirst are also experienced by some individuals. In many cases, emotional liability with panic attacks may also occur.
Paranoia and psychosis develop during thyroid storm which is characterized by an irregular heartbeat, mental agitation, and vomiting.
Even after treatment, thyroid storm results in 20% to 50% death.
Hyperthyroidism and Graves’ Disease
If Graves’ disease is the underlying cause of your hyperthyroidism, there are some additional symptoms associated with it.
It usually affects women under the age of 40. A condition called Graves’ ophthalmopathy is associated with hyperthyroidism caused by Graves’ disease. About 30% of people with Graves’ disease develop Graves’ ophthalmopathy. It affects your eyes and vision and muscles around them.
Some of its common signs and symptoms are:
- muscles behind eyeballs swells up and as a result of which they are pushed forward
- often, eye balls bulge out of their normal position
- a person will have teary eyes which are sensitive towards the light with double/blurry vision
- restricted eye movements
- pain in eyes
- redness or inflammation in your eyes
- double vision or loss of vision
Some people with Graves’ disease also develop Graves’ dermopathy, though it is rare. It causes redness and thickening of your skin, in particular, on your feet or shins.
The causes of overactive thyroid gland are largely unknown but it puts the patient at risk of developing osteoporosis and cardiovascular diseases. You may develop certain symptoms for these conditions as well.
Other Possible Symptoms
Following are other possible symptoms because of the overactive thyroid gland.
- Fatigue
- Appetite change
- Difficulty in sleeping
- Irritation
- Frequent bowel movement and sometimes diarrhea
- Light or missed menstrual periods
- Problem with fertility
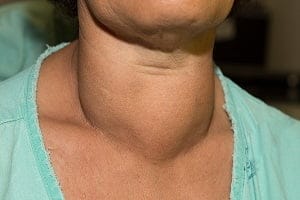
- Goitre – a swelling in neck due to enlarged thyroid gland
- Not able to concentrate
- Hair loss
- Itching
- Development of breasts in men
- Nervousness
- Loose nails
Symptoms requiring urgent attention
Certain symptoms may require immediate attention such as the following:
- Irregular heart beats
- Shortness of breath
- Dizziness
- Loss of consciousness
- Atrial fibrillation – it can be life threatening and can cause stroke or heart failure
When to see your doctor
There might be many symptoms due to a possible overactive thyroid. If you notice a few of these symptoms, it is better to meet your physician. It’s important to describe the changes you’ve observed recently, because many symptoms of overactive thyroid are similar to several other conditions.
You can try to make a list of the signs and symptoms before booking an appointment so that it helps during your interaction with him or her. Your doctor will run certain diagnosis tests to determine whether you have overactive thyroid gland. Read here about diagnosis of overactive thyroid (hyperthyroidism).
If you’ve been treated for hyperthyroidism in the past or are being treated, it’s important that you meet your doctor regularly so that your condition could be monitored.