Diagnosis of Vitiligo
- Updated on: Jun 29, 2024
- 2 min Read
- Published on Sep 27, 2019

Vitiligo is a dermatological disorder in which there is a loss of pigment (brown colour) from areas of skin, thereby causing an irregular white patch that looks like normal skin.
Difference between vitiligo and leucoderma
Vitiligo and leucoderma are two common skin disorders categorized by extensive white patches over the skin. As they both share many similar symptoms, it is usually difficult to distinguish the difference between them.
As far as the clinical presentation is concerned, both vitiligo and leucoderma consist of white patches, which can only be differentiated by the cause of their onset.
Vitiligo is a self-generated disorder, mainly caused by autoimmune conditions, hormonal changes, acute emotional trauma, and recurrent episodes of jaundice or typhoid fever, prolonged antibiotic treatments or corticosteroid therapies.
Leucoderma follows a physical trauma and is said to be accidental and can occur after a cut, a burn or after allergy from some chemical. The cure for leucoderma is faster in comparison to vitiligo.
As both the disorders differ, two clinical diagnoses are required for them. A complete medical history and physical examination of skin changes are very important to decide on the treatment plan.
The diagnosis of vitiligo can be based on the following:
Physical examination
First, your skin specialist will carefully perform a complete physical examination of the affected areas on the skin. It is mainly conducted on the sun exposed areas such as the hands, feet, arms, face and lips. Based on the patient’s examination, a preliminary confirmation is done.
Medical History
Patient’s medical history is taken if the doctor suspects vitiligo so as to confirm it and rule out other medical problems such as dermatitis or psoriasis. The doctor will enquire if the patient or any of his relatives in the family has had any autoimmune diseases and whether they have any sensitive skin after exposure to sun.
Other useful factors in diagnosis includes a rash, sunburn, stress or physical illness and premature hair graying or other skin trauma, that occurred at the site of it before the onset of depigmentation.
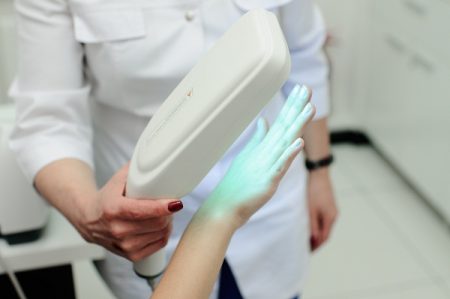
A unique light known as woods light is used by doctors to confirm vitiligo by illuminating certain suspected areas.
Laboratory Tests
- A sample of skin biopsy (of the affected skin) may be required at times to confirm the condition and rule out other possible causes of pigment loss and to examine it under a microscope. If the test is positive, the sample of skin will usually show a complete absence of pigment-producing melanocytes. In negative cases, the presence of inflamed cells in the sample may suggest that another condition is responsible for the loss of pigmentation.
- Blood tests are performed to check the levels of thyroid (such as thyroid peroxidase antibody thyroid-stimulating hormone, free triiodothyronine (T3), and free thyroxine (T4) levels) or other hormones, CBC count with differential, and vitamin B12.
- Additional blood test to check for the presence of antinuclear antibodies may also be done. Determination of another autoimmune disease can be done by these tests.
- An eye examination to check for uveitis (inflammation of parts of the eye) may be recommended in certain cases. As melanocytes are present both in the eye and in the inner ear, both ophthalmologic and auditory investigations are useful.