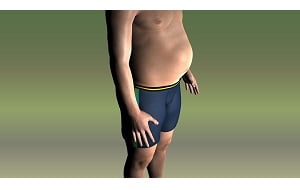
An Overview of Ascites
- Updated on: Dec 12, 2023
- 7 min Read
- Published on Nov 18, 2020

What is Ascites?
The word ascites has been derived from the Greek word ‘askos’ which means a bag or sac. Ascites is a condition characterized by an abnormal accumulation of pathologic fluid within the abdominal (peritoneal) cavity. Accumulation of more than 25 milliliters of protein-containing fluid in the abdomen is known as ascites. Ascites is caused by different diseases like cirrhosis of the liver, cancer within the abdomen, congestive heart failure, and tuberculosis. Most commonly, ascites occurs when the liver stops functioning properly. Due to the liver’s malfunctioning, an abnormal fluid fills the space between the abdominal lining and the organs, resulting in ascites.
The organs in the abdomen are enclosed in membrane or sac called the peritoneum. Normally there is a little amount of fluid within the peritoneal cavity, but in women, this fluid can vary (by 20ml or less than an ounce) depending on the menstrual cycle. Ascites is the term used to denote the increased amount of abnormal fluid in the peritoneal cavity. Various diseases result in fluid accumulation, and there are different reasons for the ascites in each condition.
Commonly, the ascites is caused due to a diseased condition like liver disease due to which the organ fails to produce enough protein to retain fluid in the bloodstream and an obstruction to flow through the scarred cirrhotic liver. Normally, the water molecules are held in the bloodstream by oncotic pressure. The protein pull keeps water molecules from leaking out of the capillary blood vessels into surrounding tissues. With the advancement in the liver disease, its ability to manufacture proteins is reduced, so oncotic pressure declines because of the lack of total protein in the body, water leaks into surrounding tissues. Apart from the ascites (abdominal ascites), the extra fluid can accumulate in many other body areas as edema (swelling) like feet, legs, chest cavity, various other organs, and fluid can get into the lungs. The symptoms of this excess fluid accumulation depend on its location.
Fast Facts About Ascites
- Ascites is a symptom of another underlying cause.
- Swelling in the Abdomen and associated weight gain are the typical symptoms of ascites.
- The prognosis and outlook of ascites depend on the underlying condition.
- Progress of the ascites can be regularly assessed by regularly measuring the abdominal girth and by monitoring weight.
What Are the Symptoms of Ascites
There is a difference between ascites caused by liver diseases like cirrhosis and ascites caused by inflammation of the peritoneum due to cancer. Ascites caused by liver disease tend to be relatively painless, while cancer patients’ ascites produce significant amounts of pain. Besides, ascites causes the swelling of the abdomen to accommodate the fluid buildup. As a result, it becomes difficult for the diaphragm to aid in breathing, resulting in shortness of breath.
The presence of small amounts of fluid in the abdomen usually causes no symptoms, moderate amounts may increase the person’s waist size and cause weight gain, but massive amounts may cause abdominal distention (swelling) and discomfort. The abdomen feels stiff, and the navel is flat or even pushed out. The swollen abdomen puts pressure on the stomach, leading to loss of appetite and pressure on the lungs, leading to shortness of breath. In some people with ascites, there occurs swelling in ankles due to accumulation of fluid there, resulting in edema.
Mostly ascites is accompanied by a feeling of fullness, a ballooning belly, and rapid weight gain. Some other symptoms often include:
- Shortness of breath
- Nausea
- Swelling in legs and ankles
- Indigestion
- Vomiting
- Heartburn
- Loss of appetite
- Fever
- Hernia
What Causes Ascites?
There are many underlying causes of ascites, among which liver disease is one of the most common reasons. Ascites typically begin due to an abnormality in the liver. A malfunctioning liver cannot make enough protein to maintain oncotic pressure to keep fluids in the circulatory system. Although the exact mechanism of ascites is unknown yet, the following conditions have a critical role in disease development.
Liver Cirrhosis
Cirrhosis is a form of liver disease in which damaged liver tissue is replaced by scar tissue. The loss of liver tissue results in progressive liver failure. Some of the common causes of liver cirrhosis include alcoholic liver disease or alcoholic hepatitis, viral hepatitis B, viral hepatitis C, and fatty liver disease. All these causes can ultimately lead to acute liver failure. Acute liver failure is one of the important causes of ascites.
Budd-Chiari Syndrome
Budd-Chiari Syndrome is caused due to blockage in hepatic veins resulting in ascites, abdominal pain, and hepatosplenomegaly(enlargement of the liver and spleen).
Cancer
Metastasis of cancer to the liver is also one of the sources of ascites.
Portal Hypertension
Portal vein is a large vein that transports blood from the intestines to the liver. High blood pressure in the portal vein and its branches, called portal hypertension, is also one of the major causes of ascites.
Other Causes
Besides the causes mentioned above, there are some other causes of ascites, which include:
Heart Failure
Heart failure is the inability of the heart muscle to pump the fluid adequately within blood vessels. This causes various problems like fluid retention into the lungs and other organs, causing them to fail. This water overload causes leakage into the peritoneal cavity and, ultimately, the formation of ascites.
Nephrotic Syndrome
It is a condition where the kidneys lose most of their proteins in the urine. This, in turn, decreases oncotic pressure and results in ascites.
Pancreatic Disorders
Pancreatic disorders have been involved in ascitic fluid formation in a variety of ways. Acute pancreatitis causes fluid accumulation as a part of the inflammatory response. On the other hand, chronic pancreatitis results in malnutrition decrease total body proteins, which decreases oncotic pressure and results in the formation of ascites. Pancreatic cancer results in direct fluid loss.
Irritation of the Peritoneum
Direct irritation of peritoneum results in fluid leakage as a part of inflammation process. This irritation may be due to any malignancy (cancer) or infection.
Diseases of the Ovary
Some diseases of the ovary have been associated with ascites. Initially, ovarian cancer in women has no symptoms and is diagnosed based on ascitic fluid formation. Meigs syndrome, a benign tumor of the ovary called fibroma, is associated with ascites and pleural effusion. The ovarian tumor’s hard surface causes a significant irritation in the peritoneum, resulting in fluid leakage.
Hypothyroidism
Ascites has been found uncommonly in hypothyroidism (low thyroid function). However, ascites resolve when thyroid levels in the body return to normal.
What Are the Risk Factors for Ascites?
Cirrhosis of the liver is one of the most common causes of ascites, and both of these conditions have some similar risk factors. Some of these risk factors include hepatitis B, hepatitis C, and long-standing alcohol abuse. Some other potential risk factors related to the other underlying conditions are congestive heart failure, malignancy, and kidney disease.
What Are the Complications of Ascites?
Excess fluid accumulation in the abdominal cavity results in many abdominal pain, discomfort, and difficulty breathing. All these problems may sometimes limit a patient’s ability to eat, walk, and perform daily activities. There are many complications associated with ascites. Some of them are:
Infection
Sometimes the ascitic fluid in the gut becomes infected with bacteria. Such a condition is called spontaneous bacterial peritonitis, which usually causes fever and abdominal pain. Spontaneous bacterial peritonitis is a severe condition that is usually treated with IV antibiotics.
Fluid in the Lungs
Sometimes the ascitic fluid gets accumulated in the lungs, and this condition is called hepatic hydrothorax. This abnormal ascitic abdominal fluid fills the lung (mostly on the right side), which causes shortness of breath, cough, hypoxemia, and chest discomfort. Hepatic hydrothorax can be treated by removing the abdominal ascites by paracentesis or ascitic drain.
Kidney Failure
Worsening of liver cirrhosis can sometimes lead to kidney failure. This condition is called a hepatorenal syndrome. It is a rare but serious condition and may lead to kidney failure.
Refractory Ascites
Refractory ascites is unresponsive or intolerant to diuretic therapy, and there is no treatment for this form of ascites.
Diagnosis of Ascites
The diagnosis of ascites is usually based on physical examination and a detailed medical history to determine the possible underlying causes because ascites is often considered a nonspecific symptom for other diseases. If the ascitic fluid is more than 500ml, it can be confirmed on physical examination by bulging flanks and fluid waves performed by the doctor while examining the abdomen. An ultrasound of the abdomen may detect a small quantity of fluid.
Diagnosing the underlying conditions causing ascites is the most important part of understanding the reason for ascites’ development. Sometimes, medical history may provide information about the underlying cause and typically includes questions about the previous diagnosis of liver disease, alcohol abuse, family history of liver disease, viral hepatitis infection and its risk factors, heart failure, cancer history, and medication history.
Blood work plays an essential role in evaluating the cause of ascites. An entire metabolic panel can detect liver injury patterns, functional status of liver and kidney, and electrolyte levels. A complete blood count test is also useful in knowing the underlying cause. Due to liver dysfunctioning, coagulation (clotting) panel abnormalities (prothrombin time) may be abnormal. Sometimes the possible underlying causes of ascites cannot be determined based on the history, examination, and review of laboratory data and imaging studies. Therefore analysis of the fluid may be necessary to obtain further diagnostic data. This procedure is called paracentesis or ascitic drain, and trained physicians perform it. It involves sterilizing an abdomen area, and then with the guidance of ultrasound, a needle is inserted into the abdominal cavity to withdraw the fluid for further analysis. The analysis of ascitic fluid is done by sending collected fluid to the laboratory quickly after drainage. Typically, it involves the analysis of the number and components of white blood cells and red blood cells (cell count), albumin level, gram stain and culture for any possible organisms, amylase level, glucose, total protein, and cytology (the study of any cells in the fluid looking for malignant or cancerous cells) in the laboratory. The doctor then analyzes the results for further evaluation and determination of the possible cause of ascites.
What Are the Best Treatments Options for Ascites?
The most important step in treating ascites is to reduce salt intake in our diet. The recommended limits for salt intake are 2,000 mg or less in a day. Consulting a nutritional specialist (dietitian) can be helpful because salt content in foods is difficult to determine. Besides this, some salt substitutes that do not contain potassium can also be used.
Patients often require diuretics (“water pills”) to treat ascites. Commonly used diuretics are spironolactone (Aldactone®) and furosemide (Lasix®). These diuretic drugs can cause problems in the electrolyte balance (sodium, potassium) and kidney function (creatinine). Taking diuretics is not a substitute for reducing the salt intake. Both are needed to treat ascites.
Some other treatments include:
Paracentesis or Ascitic Drain
Paracentesis or ascitic drain removes excess amounts of fluid from the body, especially when diuretics and restricted salt diets fail to function.
Surgery
Sometimes the treatment involves placing a tube (shunt) surgically between the main vein (portal vein) and smaller veins. A radiologist places the shunt directly through the liver, thereby relieving portal hypertension and diminishing ascites. By increasing blood flow, all organs of the body are then able to perform their function properly. For example, ascites patients with improved kidney function can help eliminate excess salt (sodium) from the body and prevent the buildup of fluids.
Liver Transplant
This treatment is usually reserved for patients with very severe liver cirrhosis and liver failure.
Outlook of Ascites
The outlook and prognosis of ascites usually depend on the underlying condition. Symptoms can be managed and reduced, but it is the treatment of ascites that gives an outcome. There is currently no proper treatment for people with liver cirrhosis and a form of ascites that is resistant to diuretics (refractory ascites). However, paracentesis (ascitic drain) and shunts without a liver transplant can improve a person’s quality of life but are not believed to considerably improve long-term life expectancy.