Risk Factors for Skin Cancer
- Updated on: Jul 6, 2024
- 7 min Read
- Published on Apr 25, 2021

Risk factors are defined as various conditions and activities that may lead to a disease condition or increase chances of getting that disease. Risk factors are different for different cancer types. Some risk factors can be controlled which are basically related to lifestyle and environment but others are uncontrollable such as heredity, genetics and age of a person.
Risk factors help in identifying different situations and conditions that may lead to a disease but having at risk factor doesn’t mean to develop that disease. But, you should be aware of them and preventive measures towards these risk factors should be taken so as to avoid the disease development.
In case of skin cancers, the risk of getting them increases mostly with exposure to sunrays. People with more than one risk factor are more likely to develop skin cancer than those with less risk factors but that doesn’t mean it will not affect a person having lesser or no risk factor at all.
Various Risk Factors for Skin Cancers
Exposure to Ultraviolet (U.V.) radiation
Exposure to U.V. radiations or spending too much time in sunlight plays a major role in developing the skin cancer. People who choose to work outside and children who play outside or spend leisure time outside in the sunlight for longer times are at higher risk of developing skin cancer. The main source of U.V. radiation is sunlight and tanning beds and lamps add on to this.
The amount of U.V. radiation exposure of someone depends upon the strength of sunlight, time of exposure (prolonged and consistence or occasional) and also on whether the skin is covered with clothes or sunscreen or not. Studies showed that people who are exposed to sunlight for prolonged period during their young age are at more risk of getting skin cancer.
The U.V rays makes a small portion of sunlight but it damages the skin and causes skin cancers to a great extent by damaging the DNA of gene controlling the growth and development of skin cells ultimately leading to DNA damage of skin cells.
U.V. rays consist of two radiation types – A and B and the U.V. type B is considered as linked to skin cancer. U.V. type B causes sunburn and is not able to penetrate car glasses. But U.V type A can penetrate car glasses and in addition to skin cancer, it mostly causes aging and wrinkling of our skin, thus playing vital role in developing skin cancer too.
It is believed that the people who live at high attitude are at great risk of getting skin cancer as they are outside most of the time and are exposed to sunlight for longer time period during their lifespan.
The nature of U.V. rays exposure plays a role in developing skin melanoma in different parts of our body, e.g. sunburn especially in childhood is linked to trunk and leg melanoma.
Many people like to tan their bodies but tanning is a skin cells response to damage from excessive U.V radiations. So, use of tan beds and lamps for tanning purposes prove harmful to skin and causes skin cancer.
Avoiding the sunrays and prolonged sun exposure alone can save life of people and protect them from getting skin cancers.
Fair Skin Tone
Skin cancer can happen to anyone regardless of complexion, race and ethnicity. But it is seen that people with light skin tone have less melanin pigment on their skin to protect from harmful U.V. radiation and they are more prone to develop skin cancer. Even people with blonde, red hairs and light colour eyes and who can sunburn easily are much likely to get skin cancer. People with light skin tones usually burns due to sunlight rather than getting tan as melanin is lesser in them.
It is estimated that white people are at higher risk of skin cancer than African Americans.
Genetics and Hereditary
People who have a family history of skin cancer such as one of the parents or siblings having skin cancer are at high risk of getting skin cancer. It is estimated that around 10% of people with melanoma have a family history of the skin cancer.
The cause of increased risk due to family history is due to family lifestyle (outdoor activities and sun exposure frequently), certain genetic defects (mutation) that may be inherited in family or may be a combination of these factors.
Most of the physicians do not advice people with family history of skin cancer to get their genetic testing as the relation of genetic heredity to skin cancer is not so clear, although it is advised for these people to take certain preventing cares such as protect their body from prolonged sun exposure, do frequent self skin examination or notice any skin aberrations by them and also by a dermatologist.
Some rare inherited genetic conditions are linked to increased risk factor for getting basal cell carcinoma such as Nevoid Basal Cell Carcinoma Syndrome also known as Gorlin Syndrome and also very rare genetic conditions such as Epidermolysis bullosa simplex syndrome, Rombo, and, Bazex-Dupré-Christol.
The rare genetic conditions such as Pigmentosum albinism, multiple self-healing squamous epitheliomata, dyskeratosis congenital and Epidermolysis bullosa simplex are linked to increased risk of developing Squamous cell carcinoma.
There is also a rare genetic inherited disease called as Xeroderma Pigmentosum in which skin’s ability to repair U.V. damage is affected and thus it increases the risk of developing skin cancers.
Moles on Body
A mole is also known as Nevus and is usually benign in nature. Moles often develop or begin to develop or appear when a child gets young or adult. Moles are not found on babies’ body naturally. Most of the moles are harmless and never cause any problem or develop into cancers. But having larger number of moles on the body may increase the risk of developing skin cancers.
People who have larger moles and abnormal moles on body called as dysplastic nevi are at risk of developing skin cancer. The dysplastic moles look abnormal and are generally larger and irregular than normal moles. These moles are more likely to develop into cancerous forms. The presence of such moles on our body may increase the chances of getting skin cancer to about 10%. Although, a small proportion of these moles may develop into melanoma but a person with these moles should regularly visit the doctor for thorough skin examination.
A rare genetic condition called as Dysplastic nevus syndrome is an inherited genetic disease and if people with this condition have any close relative suffering from melanoma, they are observed for risk of skin cancer.
Some moles are present at birth on a baby’s body called as congenital melanocytic nevi. The rate of congenital melanocyte nevi developing into melanoma is very less i.e. between 0-10% which also depends on the size of the nevus as people with large congenital melanocyte nevi are at higher risk of getting melanoma than those with small congenital nevi. The nevi are removed by surgery depending on its size, colour and location so as to avoid the chance of it to become cancerous. Doctors advise for regular self-examination and to be checked by a dermatologist if congenital nevi are not removed in a person.
Precancerous Condition of Skin
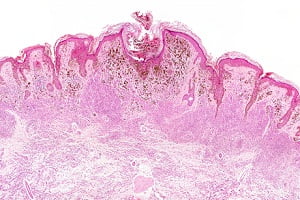
People with precancerous skin conditions such as skin lesions called as actinic keratoses, which appear as red or brown scaly patches on skin, rough and ranging in colour from dark pink to red to brown, are at high risk of developing skin cancer. These lesions appear generally on face, hands and head in people who have severe sun damaged skin or fair toned skin. These actinic keratoses usually lead to the development of squamous cell carcinoma.
The presence of more numbers of actinic keratoses increase the risk of developing squamous cell carcinoma. The use of sunscreen with sun protection factor 30 which protects from both UVA and UVB throughout the year decreases the risk of developing skin lesions or actinic keratoses.
Certain long term and severe skin conditions like skin damage from skin diseases, skin on infected bone and scars from severe burns are more likely to develop into skin cancer but this condition is very rare and risk is very less.
Suppressed or Weak Immune System
People with weak immune system due to certain disease condition such as HIV/AIDS or due to the effect of immunosuppressive drugs given in organs, bone marrow or stem cell transplantations are at risk of developing non-malignant skin cancers (basal and squamous cell carcinomas). The skin cancer tends to grow faster in immune-suppressed people than in normal personal and is likely to be fatal.
Pre-history of Skin Cancer
People with an early history of skin cancer are more likely to develop it again during their lifespan. A person who has previously been diagnosed with skin cancer is at an increased risk of getting it again. Even previous history of basal and squamous cell carcinoma increases the risk of getting melanoma in a person. Around 35-50% people who are diagnosed with one basal cell carcinoma are recorded to develop another skin cancer within 5 years.
Radiation Treatment and Therapies
Radiation treatment increases chances of developing skin cancer in people. A person who has gone through radiation treatment or therapy is at high risk of developing skin cancer, in particular, basal cell carcinoma on exposed areas.
Radiation treatment is given to treat cancer conditions and eczema. The chances of developing it increase especially after 10-20 years of the treatment. Children who receive radiation treatment have chances of developing basal cell carcinoma 6 times higher than normal children.
Psoriasis
Psoriasis is a lifelong inflammatory skin disease which is treated with psoralen and U.V. light (PUVA). It increases the risk of developing squamous cell carcinoma and other skin cancers.
Age
The risk of skin cancer increases with age due to longer time of exposure of skin to the sun. Basal cell and squamous cell carcinomas are more likely to start developing after the age of 50. But younger people may also get it due to more time spend in the sun without protection. Frequent sun burns that occur especially during childhood may increase the risk of developing melanoma particularly to fair skin tone people. Genetic skin cancer that runs in families occurs in early childhood in a person.
Gender
It is observed that men are more prone to develop skin cancers than women. Men have higher rate of melanoma than women in the U.S and this varies with age. The risk is higher for female before 50 and for male after 50 years of age.
Men are twice likely to develop basal cell carcinoma and thrice squamous cell carcinoma than women.
Chemical Substances
Exposure to certain harmful chemicals like arsenic which is used as insecticides and found in well water in areas with high arsenic use in agricultural purpose increases the chances of developing non-malignant skin cancers. Heavy metal exposure, industrial tar, paraffin, certain oils and coal also contribute in increasing risk factor for non-melanoma cancer development.
Human Papilloma Virus (HPV) Infection
A small proportion of skin cancer is linked with virus infection especially those that affects the genital areas. One of such viruses is HPV which is a group of virus causing warts. Warts generally develop around anus and in genital areas and cause skin cancer in these areas. Individuals affected with this virus have high risk of developing Kaposi sarcoma.
Sexual activity with someone having this virus affects the person too and the virus also suppresses immune system of that person thereby increasing rate of getting the cancer. A person with HPV infection is at higher risk of getting squamous cell carcinoma.
Smoking
It is observed that smoker especially regular smokers are more likely to develop squamous cell carcinoma mainly on lower lips.
Medications
Medications such as certain steroids that make skin sensitive to sunlight and prone to sunburns-vemurafenib (Zelboraf), voriconazole (Vfend ) and vandetanib (Caprelsa), increases the risk of squamous cell carcinoma. BRAF inhibitors such as vemurafenib, dabrafenib (Tafinlar)andencorafenib increase risk of squamous cell carcinoma by turning on the growth pathway of precancerous cells in a person.