How Serious Is Osteomyelitis?
- Updated on: Jul 1, 2024
- 5 min Read
- Published on Oct 3, 2019
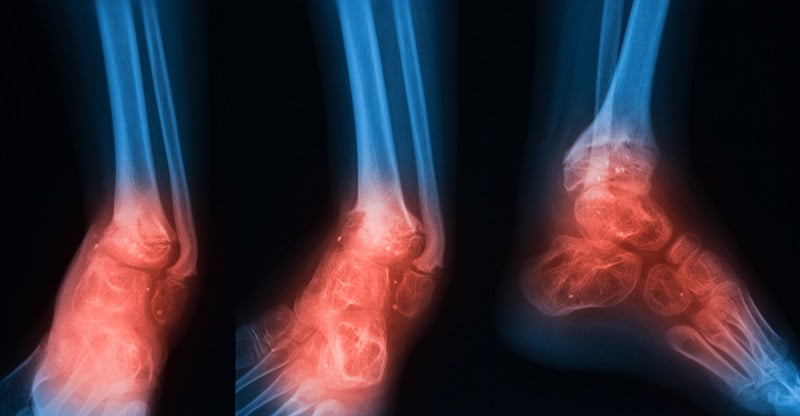
Osteomyelitis is a bone infection that can arise from germs traveling through the bloodstream, spreading from adjacent tissues, or from direct exposure due to an injury. Individuals with chronic conditions like diabetes or kidney failure, as well as smokers, face higher risks of osteomyelitis. Particularly, diabetics with foot ulcers are more susceptible to developing this infection in their feet.
Can osteomyelitis be fatal?
Osteomyelitis is a serious condition and if it is left untreated, the infection can advance to other joints and other parts of the body. This will lead to widespread infection and septic and even bone death by affecting the blood circulation within the bone.
Your doctor will need to amputate the infected bone and tissue surrounding it to check the further spreading of the infection leading to severe disability.
Infection from bone may transfer to blood and can cause blood infection resulting in blood poisoning (septicaemia) fatal illness and multiple organ failure.
In some cases, chronic infectious draining sites and the surrounding skin can evolve into a squamous-cell type of skin cancer.
In recent studies, serious neurological complications secondary to abscess have been reported associated to spinal osteomyelitis.
More: Bone Cyst: Types, Symptoms, Causes, Diagnosis, Treatment, Surgery
More: Jawbone infection (Osteomyelitis in Jawbone) Symptoms, Causes, and Treatment
Can osteomyelitis lead to death?
Osteomyelitis can be cured if treated early. In case of chronic infection, prognosis may take time and sometime amputation is the last resort.
Mortality rates associated with it are generally low unless there is a presence of chronic or serious concomitant illness.
Deaths are very rare and were common before commencement of antimicrobial regimen. Sometime, it happens in patients who have osteomyelitis of spine for a long time, due to infection of membranes surrounding the spinal cord and brain.
Osteomyelitis is a serious and potentially life-threatening condition that affects the bones and surrounding tissues. It is a bone infection caused by bacteria or fungi that can lead to bone destruction, chronic pain, and other complications if left untreated. Osteomyelitis can occur in any bone in the body, but it is most commonly found in the long bones of the arms and legs, as well as in the vertebrae and the pelvis.
Osteomyelitis is a relatively rare condition, but it can affect people of all ages and backgrounds. According to the Centers for Disease Control and Prevention (CDC), there are approximately 70,000 cases of osteomyelitis in the United States each year. The condition is more common in men than in women, and it is more prevalent in individuals over the age of 50.
Severity of Osteomyelitis
Types of osteomyelitis:
There are two main types of osteomyelitis: acute and chronic. Acute osteomyelitis develops rapidly and is typically characterized by severe pain, swelling, and fever. Chronic osteomyelitis, on the other hand, develops more slowly and can last for several months or even years. It is often associated with the formation of bone abscesses and chronic draining sinuses.
Causes of osteomyelitis:
Osteomyelitis can be caused by a wide range of bacteria and fungi, but the most common cause is Staphylococcus aureus. This bacterium is found on the skin and in the nasal passages of many healthy individuals, but it can cause infections if it enters the body through a wound or surgical incision. Other causes of osteomyelitis include tuberculosis, osteoporosis, and bone tumors.
Symptoms of osteomyelitis:
The symptoms of osteomyelitis can vary depending on the type of infection and the location of the affected bone. However, some common symptoms include pain and tenderness in the affected area, swelling and redness, fever, chills, and fatigue. In some cases, the infected area may also be warm to the touch and may produce pus or other discharge.
Diagnosis of osteomyelitis:
Diagnosing osteomyelitis typically involves a combination of physical exams, imaging tests, and laboratory tests. X-rays and other imaging tests can help identify changes in bone density and bone structure that are characteristic of osteomyelitis. Blood tests can also be used to detect signs of infection, such as elevated white blood cell counts and increased levels of inflammatory markers like C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR). In some cases, a biopsy of the affected bone tissue may also be needed to confirm the diagnosis.
Complications of Osteomyelitis
Osteomyelitis is a serious condition that can lead to a range of complications if left untreated.
Some of the most common complications of osteomyelitis include:
- Bone necrosis: This occurs when the infected bone tissue dies and can no longer support the surrounding bone structure. In severe cases, bone necrosis can lead to bone fractures and deformities.
- Joint infection: Osteomyelitis can spread to the joints, leading to inflammation, pain, and reduced mobility. In some cases, joint infection may require joint replacement surgery.
- Sepsis: This is a potentially life-threatening complication that occurs when the infection spreads to the bloodstream. Sepsis can cause organ failure, shock, and even death if not treated promptly.
- Amputation: In rare cases, osteomyelitis can lead to such severe bone and tissue damage that amputation may be necessary to prevent the spread of infection.
Treatment of Osteomyelitis
Early diagnosis and prompt treatment are essential for managing osteomyelitis and preventing complications. Treatment options for osteomyelitis may include:
- Antibiotics: Depending on the type and severity of the infection, antibiotics may be prescribed orally or administered intravenously. Antibiotics are typically used to control the spread of infection and to prevent further bone damage.
- Surgery: In cases of severe or chronic osteomyelitis, surgical intervention may be necessary to remove infected tissue and promote healing. Surgical options may include debridement (removal of dead or infected tissue), bone grafts (replacement of damaged bone with healthy bone tissue), or amputation (in extreme cases).
- Pain management: Osteomyelitis can cause severe pain and discomfort, and effective pain management is an important part of treatment. Pain medication, physical therapy, and other non-invasive treatments may be used to help manage symptoms and improve quality of life.
Prevention of Osteomyelitis
Preventing osteomyelitis is crucial as it is a severe and life-threatening condition.
Here are some ways to prevent osteomyelitis:
- Proper wound care: Wounds are the primary way that bacteria enter the body and cause osteomyelitis. Proper wound care is essential to prevent the development of the condition. It involves cleaning the wound, keeping it dry, and covering it with a sterile dressing.
- Managing chronic conditions: Individuals with chronic conditions like diabetes and peripheral artery disease are at a higher risk of developing osteomyelitis. Proper management of these conditions can help reduce the risk of developing osteomyelitis. It is essential to manage blood sugar levels and maintain a healthy weight.
- Good hygiene: Maintaining good hygiene is crucial to prevent the spread of infection. This includes washing your hands regularly, avoiding close contact with people who are sick, and not sharing personal items like towels or razors.
Prognosis and Follow-Up
The prognosis for osteomyelitis depends on several factors, including age, the severity of the infection, and any underlying medical conditions. Early diagnosis and prompt treatment of the infection are critical for improving the prognosis.
Proper follow-up care is also necessary to ensure that the infection does not recur. Individuals who have had osteomyelitis in the past must be vigilant about any signs of the infection and seek prompt medical attention if needed. They must also take steps to prevent future infections by maintaining good hygiene, managing chronic conditions, and avoiding injuries.
Overall, preventing osteomyelitis requires careful attention to wound care, chronic condition management, and hygiene. Maintaining good health habits and seeking prompt medical attention when needed can significantly reduce the risk of developing this serious condition.










1 Comment
Nausea, headache, dizziness, insomnia, anxiety, nervousness or infection, and skin reactions that can become permanently disabling, disfiguring, and life threatening.