Postmenopausal Ovarian Cyst and Malignant Ovarian Cysts
- Updated on: Jul 13, 2024
- 3 min Read
- Published on Oct 3, 2019
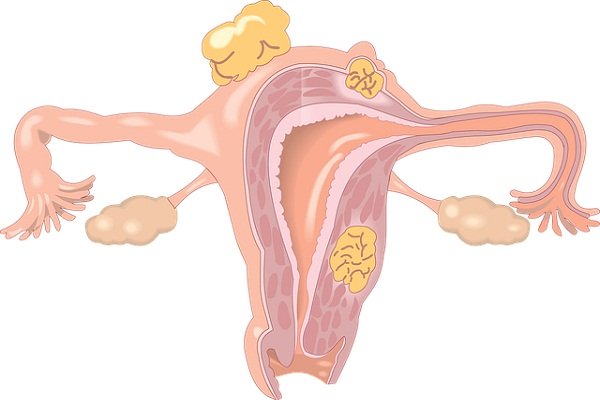
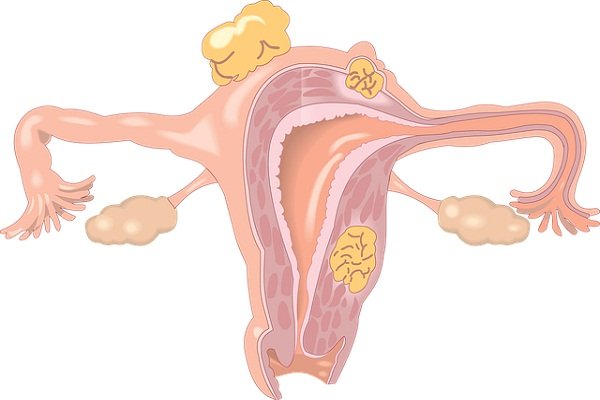
Do cysts go away after your period?
Majority of cysts never gets noticed and resolves without the woman even noticing that they had cysts in the ovary. Most cysts dissolve and disappear on their own after several menstrual cycles.
It is logical to think that when you stop having periods, chronic conditions of your female reproductive organs will also go away or stop. But that isn’t necessarily true. You may have endometriosis, fibroids and polycystic ovary syndrome even after menopause.
Are ovarian cysts common in menopause (Ovarian cyst after menopause)?
Ovarian cysts are more common in premenopausal women than post menopausal women. But, ovarian cysts in post-menopausal women are now known to be very common after menopause.
Women with ovarian cysts are at higher risk for ovarian cancer and other complications. Since age is a risk factor for ovarian cancer, any cysts in a postmenopausal woman should be taken seriously.
Before menopause, most women have ovarian cysts at some point in their lives. However, estimated 14-17% of postmenopausal women also develop cysts, so although the risks are smaller, cysts are still possible. Read about Ovarian Cysts, Causes, Symptoms, Diagnosis, and Treatment.
There is also a small chance that a cyst could be cancerous, in post menopause women. Therefore, it’s good to know about the symptoms of ovarian cysts in order to know when to see a doctor. The most common symptoms include:
- Sudden pain in the lower abdomen
- Swelling or bloating of the abdomen
- Pain in lower back, thighs and pelvis
- Pain with nausea and vomiting
- Weakness, dizziness and fever
- Rapid breathing
More: Ovarian Cyst Pain Relief: What Can I Do For Ovarian Cyst Pain?
More: Ovarian Cyst During Pregnancy: How Do Ovarian Cysts Affect Pregnancy?
Malignant Ovarian cysts
Ovarian cancer risk increases after menopause; this is why all postmenopausal ovarian growths are carefully checked for signs of cancer and sometimes doctor recommends to remove the ovaries (oophorectomy) after menopause if there is any cyst development.
Generally, for 5 years after menopause, some women will still have functional ovarian cysts now and then. Some postmenopausal women develop ovarian cysts called unilocular cysts, which have thin walls and one compartment. But these are rarely linked to cancer.
A comprehensive evaluation should be made by a physician and an expert in a pelvic ultrasound with A CA125 blood test for all post-menopausal women with ovarian cysts. Simple cysts containing only liquid are generally benign and may be followed for wait and watch. If the cyst is associated with elevated levels of CA125 and pain, removal of ovary should be considered.
Complex cysts which have potentially malignant characteristics should thoroughly be evaluated in a pelvic imaging examination, and careful consideration about their removal should be discussed.
More: Ovarian Cyst Removal And Ovarian Cyst Surgery
Can ovarian cysts be cancerous?
Studies have revealed that benign ovarian cysts do not turn into cancerous cysts, so if you have an ovarian cyst that seems to be benign upon diagnosis, waiting for it to go away for two months or so is not risky.
Numerous researches have also shown that women who form benign ovarian cysts and those women who have had no cysts are equally likely to develop ovarian cancer.
Females who are not ovulating like a woman after menopause or a girl who hasn’t started her periods are at greater risk that an ovarian cyst in these women can be concerning. Various diagnostic approaches should be employed if the cyst is large or if it does not go away in a few months. Even though most of these cysts are benign or not cancerous, a small number of them could also be cancerous.
Sometimes surgery is the only way to take out the cyst and confirm whether it’s cancerous or not. Based on how they look on imaging tests, cysts that appear to be benign can be observed and removed with surgery.
What are the symptoms of a cancerous ovarian cyst?
A pelvic mass which also includes an ovarian cyst can be benign or malignant in nature. Like benign ovarian cysts, cancerous tumours sometimes cause no or only minor symptoms at first. Symptoms of the ovarian cancer are similar to an ovarian cyst, tumours or extra masses. The symptoms may include:
- Pelvic pain
- Nausea or vomiting
- A dull ache in the lower back and thighs
- Difficulty emptying your bladder
- Pain shortly before or after the start of your period
- Pressure, swelling or pain in the abdomen
- Pain during sex
- Abnormal bleeding
- Frequent urination
If you are experiencing any of these symptoms, you should consult your doctor as soon as possible.












