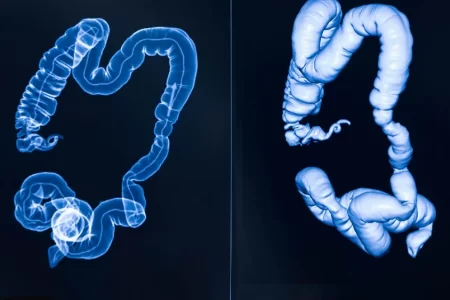
Causes of Diverticulitis
- Updated on: Jul 10, 2024
- 3 min Read
- Published on Sep 26, 2019
Diverticulitis is a digestive tract condition in which bulging sacs from the lining of colon get acutely infected and inflamed. The most common symptom of this disease is a sudden pain in lower abdomen. Normally, a diet rich in fiber and drinking adequate amount of water can prevent this condition.
To pass out hard and small stool from the body, colon (large intestine) has to exert more pressure than usual. In addition, a diet low in fiber increases the time stool remains in the bowel. This adds on to strain on the intestinal wall.
Pouches or sacs may be formed when high pressure pushes against the inner wall of the colon. Some people having these diverticula develop diverticulitis while others do not.
What causes diverticulitis?
The exact reasons for developing diverticulitis are not known, but eating a low fiber diet is thought to impact the formation of sacs in the colon as it causes constipation.
Constipation, in other words, means to apply more pressure in order to pass out stool. A decrease in healthy bacteria and an increase in disease-causing bacteria in the colon may also lead to diverticulitis.
Following are the main causes of diverticulitis:
- Constipation and hard stool
- Overweight and obesity
- Aging
- Family history
Doctors say that an increased pressure on the colon leads to the formation of pouches that later get infected and inflamed. Diverticulitis may begin when bacteria or stool get caught in pouches developed in the large intestine. This disease is irreversible in nature.
Constipation and Hard Stool
A research reveals that women are more likely to get affected by diverticulitis as constipation affects more women as compared to men. Constipation exerts pressure on muscles during the bowel movement.
Constant pressure can increase the chances of developing diverticula in the large intestine. Once sacs or pouches develop in the large intestine, they are likely to get infected and inflamed by bacteria present in stool which leads to diverticulitis.
People who have hard stool but are not constipated are also at risk. A hard stool (large or small) has nothing to do with the regularity of motion but with the strain exerted on the walls of the colon. Read about symptoms of diverticulitis.
Overweight
A study suggests that having a high Body Mass Index (BMI) and waist circumference contributes to the formation of diverticula. Obesity increases the risk of diverticulitis.
Aging
In addition to gray hair, menopause and wrinkles, there is more to growing age. Often people over the age of 50 years are likely to suffer from diverticulitis. This may be due to the weakening of bowel movement with time.
Family History
Having a family history of diverticulitis increases the risk of a person to develop this digestive tract condition. Though this has nothing to do with genes but when we share the table, we also share food habits. The fooding-habits are carried forward to adulthood and may result in digestive problems.
Other factors
In addition to obesity and constipation, other factors may also result in the development of diverticulitis like:
- Smoking
- Lack of exercise
- High animal fat and low fiber diet
- Medications like steroids, opiates and nonsteroidal anti-inflammatory drugs (ibuprofen and naproxen)
Am I at risk for diverticulitis?
Diverticulitis largely depends on persons eating habits and bowel movement. Persistent constipation and hard stool are a result of low fiber diet and not drinking plenty of water. Following people are at increased risk of developing diverticulitis:
- people who smoke
- people who eat processed food more
- people having a low-fiber diet
- people doing less of physical activity or living a sedentary lifestyle
Eating fresh vegetables and fruits (along with bran products) greatly help in pressure-free bowel movement. At least five servings of fruits and vegetables along with beans and whole grains should be taken on a daily basis to avoid digestive conditions like diverticulitis.