Nipah Virus (NiV) Disease: Symptoms, Prevention, and More
- Updated on: Jul 5, 2024
- 4 min Read
- Published on Apr 22, 2021

What is Nipah virus (NiV) infection?
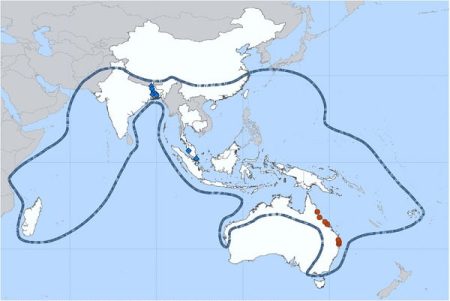
Nipah virus (NiV) infection is a newly emerging disease that can cause severe problems in both animals and humans. The natural host of Nipah virus are fruit bats of the Pteropodidae Family, Pteropus genus.
Facts about Nipah virus
- Nipah virus is an RNA virus that is part of the Paramyxovidae family and was first identified after an outbreak causing respiratory illness in pigs and encephalitic disease in humans in Malaysia and Singapore in 1998 and 1999.
- Nipah virus can cause many diseases that can range from mild to severe in domestic animals.
- In humans, Nipah virus infection can cause a range of diseases ranging from asymptomatic infections to acute respiratory infection and life-threatening encephalitis.
- The virus can be transmitted to humans from animals (such as from bats and pigs)
- The virus can also be transmitted directly from human-to-human.
- Fruit bats of the Pteropodidae family are the natural host of Nipah virus.
- There is no treatment or vaccine for either people or animals infected with the virus till date. The primary treatment of the infection for humans is supportive care.
- WHO has listed Nipah virus in its list of Blueprint priority diseases
When was Nipah first identified?
Nipah (NiV) was first identified during an outbreak of disease that took place in Kampung Sungai Nipah, Malaysia in 1998. Pigs were found to be the intermediate hosts in this outbreak. But, in subsequent NiV outbreaks, there were no intermediate hosts. It was then found in Bangladesh in 2004, when humans became infected with Nipah virus as a result of consuming date palm sap that was contaminated by infected fruit bats.
Causes and transmission of Nipah virus infection: Can Nipah be transmitted from human to human?
Human-to-human transmission of Nipah virus has also been documented. A case of human to human transmission has been recording in a hospital setting in India among others.
In the Bangladesh and India outbreaks, consumption of fruits or fruit products (such as raw date palm or their juices juice) contaminated with urine or saliva from infected fruit bats was the most common source of infection.
There are cases where some level of human to human transmission of NiV has also been reported among family and care givers of infected patients.
As found in the outbreaks in Bangladesh and India, Nipah virus spread directly from human-to-human through close contact with people’s secretions and excretions.
How does Nipah virus spread?
Transmission of Nipah virus can occur in the following ways:
- Direct contact with infected bats
- Direct contact with infected pigs
- Direct contact with other NiV infected people.
- Person-to-person transmission of Nipah virus
- Consumption of fruits such as raw date palm sap contaminated with infectious bat excretions or secretions
Signs and symptoms of the Nipah virus infection
Infections in humans may range from asymptomatic infection to acute respiratory infection and fatal encephalitis. Commonly observed initial signs and symptoms of Nipah virus infection are similar to influence, such as:
- Fever
- Headaches
- Myalgia (muscle pain)
- Vomiting
- Sore throat
Later, the infected person may develop these symptoms:
- Dizziness
- Drowsiness
- Neurological problems indicative of acute encephalitis
- Atypical pneumonia
- Severe respiratory problems such as acute respiratory distress
- In severe cases, encephalitis and seizures can occur, which can progress to coma within 24 to 48 hours.
Diagnosis of Nipah virus infection
Initial signs and symptoms of the infection are not specific and usually the infection is not suspected. This often creates challenges in diagnosing the infection and preventing outbreaks.
NiV infection can be diagnosed by studying clinical history. The tests that are often used include real time polymerase chain reaction (RT-PCR) from bodily fluids and as antibody detection via ELISA. Other tests for the diagnosis of Nipah virus infection are:
- enzyme-linked immunosorbent assay (ELISA)
- virus isolation by cell culture
- polymerase chain reaction (PCR) assay
Treatment of Nipah virus infection
Currently, there is no drug or vaccine to cure Nipah virus infection even though this is a priority disease, identified by WHO. Major complications that occur in the severe cases involve respiratory and neurologic complications, which are usually managed with intensive supportive care.
The drug ribavirin has been shown to be effective against the viruses in vitro, but human investigations to date have not been conclusive and the clinical usefulness of ribavirin is not confirmed.
Passive immunization using a human monoclonal antibody targeting the Nipah G glycoprotein has been studied in the post-exposure therapy in the ferret model and found to be of benefit.
Prevention of Nipah virus infection in humans: How can you reduce the risk of infection in people?
Since there is no licensed vaccine for the infection, the only way to reduce the risk of infection in people is by raising awareness of the risk factors and educating people about the measures that can be taken to reduce an exposure to the Nipah virus and decrease the chances of spread of the infection.

These are important considerations to help prevent the infection:
Reducing the risk of bat-to-human transmission
- Prevention of the virus transmission should be done by decreasing bat access to fruits and fruit products that cause spread of the infection such as date palm sap and to other fresh food products.
- Keeping bats away from these fruits and fruit collection sites may be helpful.
- Fresh date palm juice should be boiled.
- Fruits should be properly washed and peeled before consumption.
Reducing the risk of animal-to-human transmission
- Wear gloves and other protective clothing while handling sick animals or their tissues
- Wear gloves and other protective clothing during slaughtering and culling processes.
- Avoid being in contact with infected pigs as far as possible
Reducing the risk of human-to-human transmission
- Avoid close unprotected physical contact with Nipah virus-infected people
- Practice regular hand washing after caring for or visiting sick people
- Health-care professionals who provide care for patients suspected or confirmed with NiV infection should implement standard guidelines and infection control precautions for themselves and for all patients
- Contact and droplet precautions should be used along with standard precautions as human to human transmission has been reported.
Survival, Recovery, Death
The incubation period is defined as time interval from infection to the onset of symptoms. In case of Nipah virus infection, the incubation period is considered between from 4-14 days. However an incubation period as long as 45 days has been reported in some cases.
Most people who survive acute encephalitis are able to fully recover. But there are cases where long term neurologic conditions have been reported in survivors of the infection.
According to data obtained from WHO, approximately 20% of patients are left with residual neurological consequences such as seizure disorder and personality changes. A small number of people who recover subsequently relapse or develop delayed onset encephalitis.
Fatality rate is estimated about 40% to 75%; however. Latent infections with subsequent reactivation of Nipah virus and death can occur months and sometimes even years after the exposure.