Unilateral vs Bilateral Retinoblastoma: What is Bilateral Retinoblastoma and how is it treated?
- Updated on: Jul 9, 2024
- 3 min Read
- Published on Apr 21, 2019
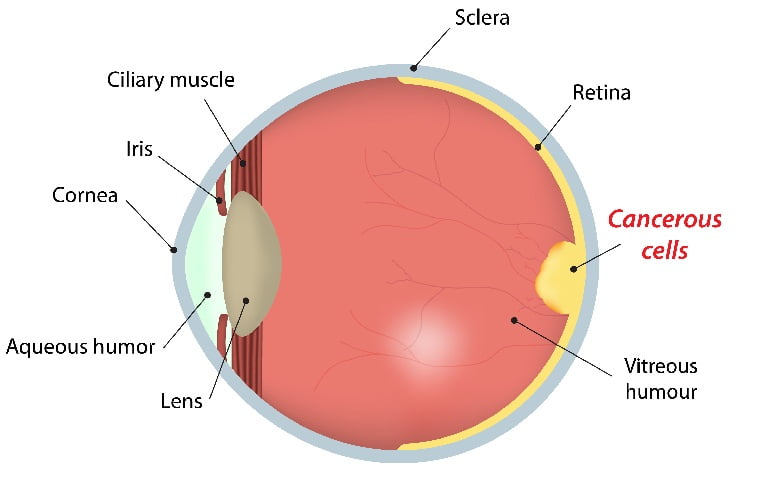
What Is Retinoblastoma?
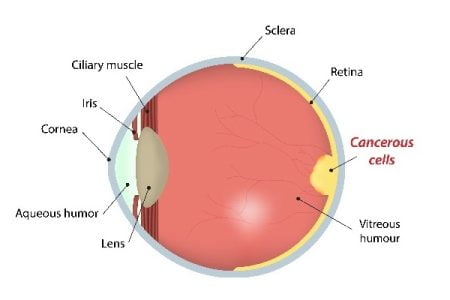
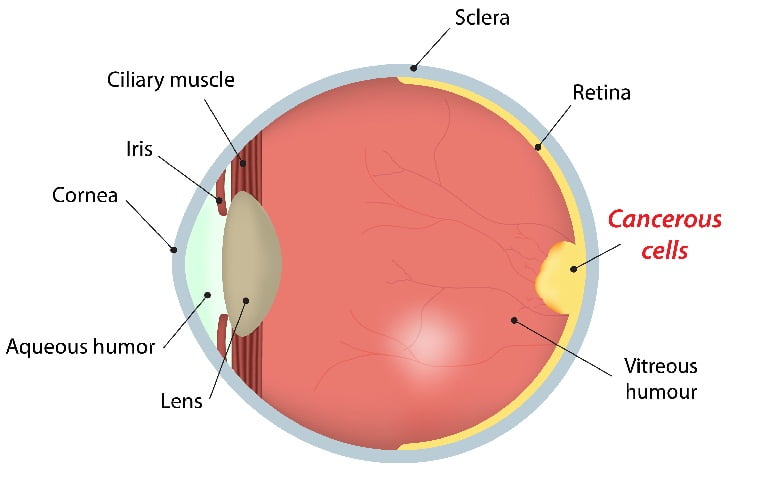
Retinoblastoma is a cancer that originates in the retina of your eye. Retina is located at the back part of the eye. Retinoblastoma is the most common type of eye cancer in children.
Read about eye cancer.
What is bilateral retinoblastoma? What is unilateral retinoblastoma?
In children, retinoblastoma can occur in one or both of eyes. When the condition occurs in only one eye, it is called unilateral retinoblastoma. The term “unilateral” stands for “one side.”
When the eye cancer is present in both the eyes, the condition is called bilateral retinoblastoma. The term “bilateral” stands for “two sides.”
Blateral retinoblastoma is generally present at an earlier age than unilateral retinoblastoma. It is estimated that about 60% of pediatric retinoblastoma cases are unilateral, and the remaining are of bilateral retinoblastoma.
The cancer does not spread from one eye to the other in bilateral retinoblastoma. When both eyes are affected and / or multiple tumours form, each tumour arises from a unique retinal cell.
More: Eye Cancer (Ocular Cancer) Causes, Symptoms, Types, Stages, Risks, Treatment, Prevention
Genetics of unilateral and bilateral Retinoblastoma: Can you inherit retinoblastoma?
Pediatric retinoblastoma (retinoblastoma in children) can be inherited by children from one or both parents. Such a cancer of eye is called hereditary retinoblastoma. If the cancer is not inherited from any of the parents, the retinoblastoma is termed as non-hereditary retinoblastoma.
Most bilateral retinoblastoma cases are also hereditary. And, the majority of unilateral retinoblastoma cases are non-hereditary. Non-hereditary retinoblastoma is sometimes referred to as sporadic retinoblastoma.
All cases of bilateral retinoblastoma are caused by genetic errors on the RB1 gene which may be inherited from a parent or occur during early embryo development.
Genetic testing can be done to determine whether a child is at risk and whether further eye exams are needed. 50% of babies with a known risk are born with tumours already formed.
How is the treatment for unilateral and bilateral retinoblastoma different?
Treatment of unilateral and bilateral retinoblastoma is generally different. In bilateral retinoblastoma, children have a higher tendency of developing tumors with time. Treatment of each tumor may be less aggressive.
Treatment of bilateral retinoblastoma involves focal treatments. Focal treatments are directed on shrinking tumors through treatment options such as laser therapy, cryotherapy, or brachytherapy. Chemotherapy and radiation therapy may be used for advances cases where the cancer has spread to other locations.
Retinoblastoma enucleation is a surgical procedure that involves complete removal of the eye. Enucleation is more commonly done in unilateral retinoblastoma cases than in bilateral retinoblastoma.
Bilateral retinoblastoma life expectancy (Survival rate)
It has been found that survival rate for retinoblastoma is greatest among patients diagnosed before 2 years of age or after 7 years of age.
According to a study from Harvard, children with retinoblastoma in both eyes are generally diagnosed at a younger age (about 13 to 15 months) than children with unilateral disease (about 24 months). The overall average age at diagnosis is 18 months.
If the tumor is present within the eye (whether one or both), more than 95% of patients who get proper treatment can be cured. For children with retinoblastoma in both eyes, about 70-80 percent of the cases can be cured.
Risk of secondary eye cancer
Children with bilateral retinoblastoma have a life-long risk of developing second cancers that can spread to the other parts of the body from eye. The chances of spread are increased by exposure to radiation. Therefore, it is recommended to avoid radiotherapy, CT scans and x-rays wherever possible.
High risk patients should receive genetic counseling so they understand their risks and the potential risks of passing it to their children.