Browsing: Health and Wellness
Comprehensive Information, Resources, and Support on Health and Wellness
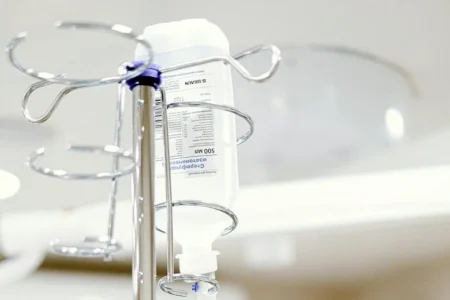
What Is IV Therapy?
IV (intravenous) therapy is a way of delivering fluids, medication or nutrients directly into the bloodstream. This allows for fast…
How Healthcare Keynote Speakers Are Shaping the Future of Preventive Medicine
A sea change is taking place in how individuals view their health. Across America, people are finding information sources that…
How to Manage Chronic Conditions With Healthy Lifestyle Choices
Living with chronic conditions can be overwhelming, but choosing a healthier lifestyle can significantly impact your daily life. Simple changes…
Aging brings a unique journey of independence that can be empowering yet also a little overwhelming at times. One concern…
Everything to Know About Building a Resilient Immune System
Have you ever thought about why some people don’t get sick often while others catch every virus going around? The…
The 80/20 Rule in Health: Focusing on What Really Matters for Long-Term Wellness
Health advice can feel overwhelming—new diets, fitness trends, biohacks, and wellness products pop up every week. But long-term wellness doesn’t…
How Community-Based Approaches Improve Health Outcomes
Healthcare has traditionally centered around hospitals, clinics, and medical offices. These spaces are designed for diagnosing and treating disease, but…
Difference Between Breast Augmentation and Breast Lift
When it comes to the improvement of body shape, breast enlargement is an excellent solution for women. The majority of…
How to Choose the Best Primary Care Provider for Your Family
When it comes to raising a family, your health is everything. So, taking care to protect it and ensuring you…
Access to Bariatric Surgery in Tennessee: Options and Eligibility
The long-term solution of bariatric surgery has become one possibility for people who deal with obesity. Weight loss through bariatric…