Multiple Sclerosis
- Updated on: Aug 6, 2024
- 6 min Read
By
- Published on Apr 19, 2021
Multiple sclerosis or MS is characterized by an immune-mediated process in which the body’s immune system directs an abnormal response against the central nervous system (CNS). The Central Nervous System is comprised of the brain, spinal cord, and optic nerves.
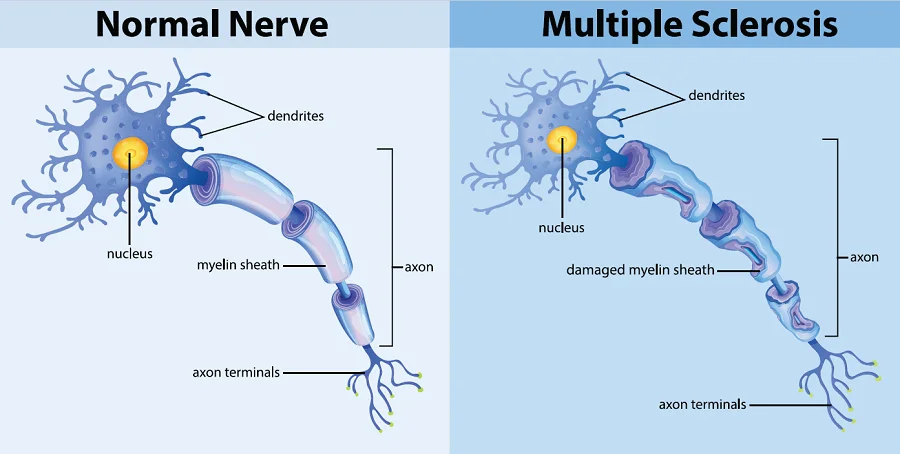
The immune system causes inflammation that damages the myelin and the nerve fibers in the brain, spinal cord, and optic nerve and the specialized cells that make myelin within the central nervous system. Myelin is the fatty substance that surrounds and protects the nerve fibers. As the attack progresses, the myelin sheath becomes inflamed and damaged gradually. As a result, patchy scar tissues disrupt the brain’s electrical impulses to other parts of the body.
Damage caused to the central nervous system may produce various neurological symptoms that may differ among people with multiple sclerosis in type and severity. The exact cause of MS is unknown, but it is believed to involve genetic propensity, an aberration in the immune system, and ecological factors that collectively trigger the disease. Most healthcare professionals believe that MS is an autoimmune condition.
The term “multiple sclerosis” refers to the multiple areas of scar tissue, usually referred to as “multiple scarring” developed all along affected nerve fibers and can be seen in MRI scans. The lesions or scars caused by Multiple sclerosis, and the resulting disturbance of nerve impulses all over the body, are what cause most of the symptoms allied with multiple sclerosis.
Symptoms of Multiple Sclerosis
The symptoms of Multiple Sclerosis are variable and unpredictable. No two people exhibit the same symptoms, and every individual’s symptoms can modify or fluctuate over time. One person might experience only one or two of the possible symptoms, while others may experience many more. Most of the symptoms can be managed effectively with medication, rehabilitation, and other management strategies.
Primary Symptoms
Primary symptoms (more and less common) of multiple sclerosis are the direct result of the myelin and nerve fibers’ damage in the central nervous system (CNS). More common symptoms associated with MS include:
- Fatigue
- Walking difficulties
- Numbness or tingling
- Spasticity
- Weakness
- Vision problems
- Vertigo and dizziness
- Bladder problems
- Sexual problems
- Bowel problems
- Pain
- Cognitive changes
- Emotional changes, depression
- Less common symptoms associated with MS include:
- Speech problems
- Swallowing problems
- Tremors, seizures
- Breathing problems
- Itching
- A headache
- Hearing loss
Secondary and Tertiary Symptoms
The secondary symptoms are the complications that can arise due to the primary symptoms associated with multiple sclerosis. For instance:
- Bladder dysfunction may lead to repeated urinary tract infections.
- Inactivity usually results in loss of muscle tone, poor postural alignment and trunk control, and decreased bone density, leading to fractures.
- Inefficient breathing
- Immobility may lead to pressure sores.
Tertiary symptoms are the effects of the disease on the life of an individual. These symptoms include social, vocational, and psychological complications. The stress and strain of dealing with multiple sclerosis usually alter social networks and cause people to withdraw from social interactions and become isolated.
Read More About Living With Multiple Sclerosis
Diagnosis of Multiple Sclerosis
Multiple sclerosis is usually diagnosed based on an individual’s history of symptoms, along with the outcome of MRI scans and several other medical tests.
Early Diagnosis of MS is critical. Early diagnosis can be beneficial as the treatment may begin early to slow down the disease’s progression. Though no single test can diagnose the disease, and multiple sclerosis symptoms imitate other conditions. Additionally, the symptoms and severity of the disease may show a discrepancy from person to person. Thus, all such conditions make a diagnosis of MS challenging.
A newly revised set of guidelines, known as the “McDonald Criteria for the Diagnosis of Multiple Sclerosis”, aimed to accurately diagnose MS in certain people with a specific indication of MS, referred to as “Clinically Isolated Syndrome.” The criteria have been refined to include new research findings, accelerate diagnosis, and avoid misdiagnosis.
Different Types of Multiple Sclerosis
At some points, inflammation is the major characteristic of the disease, but neurodegeneration can also predominate depending on the type and severity. There are several types of multiple sclerosis, including:
Relapsing-Remitting Multiple Sclerosis (RRMS)
RRMS is characterized by stages of active inflammation in the central nervous system, during which symptoms may worsen, and new symptoms may also develop.
The period when symptoms get worse is referred to as relapses, flares, or exacerbations. When a relapse ends, the severity of symptoms decreases. However, an individual can be left with new, permanent symptoms. The quiet phase between relapses is called remissions. Remissions may last for months or years before a new relapse occurs.
Secondary-Progressive Multiple Sclerosis (SPMS)
SPMS is usually considered as a secondary phase of RRMS, in which there are symptom progression and amplified disability. People associated with SPMS may suffer from persistent relapses, but they may be less frequent than RRMS.
Primary-Progressive Multiple Sclerosis (PPMS)
During the PPMS stage, there is no initial relapse that triggers the beginning of the disease. However, multiple sclerosis symptoms slowly come into sight in due course. People associated with PPMS usually do not experience acute exacerbations or distinct remissions, but they may have temporary plateaus.
Benign Multiple Sclerosis
A small number of people are associated with benign multiple sclerosis disease, in which symptoms progress very slowly after the initial attack during a person’s lifetime.
Malignant Multiple Sclerosis
A small number of people associated with malignant multiple sclerosis, which is manifested by the rapid development of lesions in the brain and spine. It can cause severe symptoms, disability, and even death.
Complications Associated With Multiple Sclerosis
Apart from the direct impact of multiple sclerosis, there is much varying severity associated with the disease, including:
Urinary Tract Infections
According to the National Multiple Sclerosis Society, urinary bladder problems are prevalent in people (affecting at least 80 percent) with multiple sclerosis.
Some people find difficulty holding their urine (incontinence), while others can’t fully empty their bladder (retention). Failing to empty the urinary bladder raises the risk of developing a urinary tract infection, causing a worsening of symptoms associated with MS.
If not treated promptly, a urinary tract infection may, in turn, lead to a kidney infection, which is a medical emergency.
Aspiration Pneumonia
If the person associated with multiple sclerosis cannot cough forcefully, the food and liquid may enter the lungs. As a result, it can lead to aspiration pneumonia. Symptoms of aspiration pneumonia may include chest pain, fever, shortness of breath, and coughing up thick, foul-smelling mucus. It is recommended to seek medical help if one experiences these symptoms.
Physical Trauma Associated With Multiple Sclerosis
Many symptoms associated with multiple sclerosis, including balance problems, muscle weakness, fatigue, dizziness, blurred vision, and numbness, increase the risk of falling. Falling may increase the risk of severe injuries (such as broken bones and head shock). Falling may also lead to a fear of falling; thus, a person may become less active and weaker.
Pressure Sores
Also known as bedsores or pressure ulcers, pressure sores are areas of damaged skin caused by applying pressure to the area for too long. People with MS who spend most of their time sitting or lying down may develop pressure sores. They tend to grow in areas where the bones are close to the skin, including heels, tailbone, shoulder blades, and elbows.
Treatment of Multiple Sclerosis
There is no cure available for multiple sclerosis, but many treatments may improve the condition and keep the body working well. Your healthcare professional may prescribe drugs that can slow the disease’s progression, prevent or treat attacks, relieve the symptoms, or aim to manage the stress associated with the disease.
Drugs that may minimize the progression of multiple sclerosis or protect against nerve damage include:
- Beta interferon (Avonex, Betaseron, and Rebif)
- Copolymer-1 (Copaxone)
- Dalfampridine (Ampyra)
- Dimethyl fumarate (Tecfidera)
- Mitoxantrone (Novantrone)
- Natalizumab (Tysabri)
- Ocrelizumab (Ocrevus)
- Teriflunomide (Aubagio)
A healthcare professional may prescribe steroids to make multiple sclerosis attacks shorter and less intensified. The doctor may also recommend certain drugs to ease muscle spasms and in treating some of the other symptoms, including:
- Muscle Relaxants
- Tranquilizers
- Botulinum Toxin (Botox)
Along with treatment, a physiotherapist may advise you to perform several exercises that can enhance the strength and balance and manage pain and fatigue. Occupational therapy can educate new ways to do a specific task easily. If you encounter difficulty while getting around, a stick, walker, or braces may help you walk more easily.
In addition to treatment, one may be able to carry out other things to ease symptoms of multiple sclerosis, including:
- Perform regular exercises
- Avoid excessive heat
- You may try yoga to alleviate fatigue or stress
- Manage emotional health (ask family, friends, or a counselor for help to overcome any stress or anxiety)
What is the Outlook for Multiple Sclerosis?
Researchers are trying to provide more specific treatment methods for the condition, a better idea of what causes it, and the ability to diagnose it as early as possible. Stem-cell and genetic research may soon help healthcare professionals to repair damaged nerves or stop the disease before it causes any damage.
Researchers looking for new ways to treat multiple sclerosis in clinical trials. The clinical trials test new drugs to see if they are harmless and how efficiently they can work to treat the disease.