Diagnosis of Shingles
- Updated on: Jun 29, 2024
- 2 min Read
- Published on Sep 27, 2019
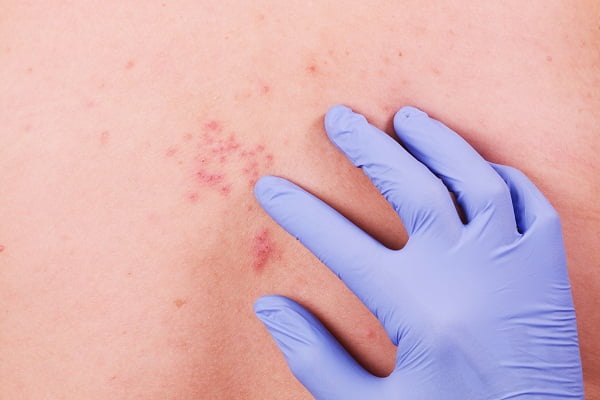
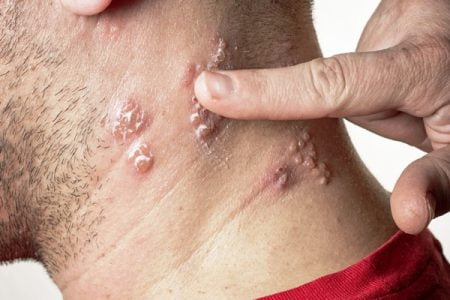
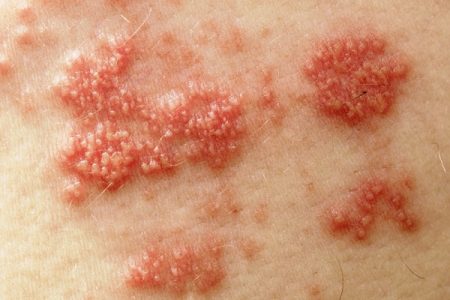
When doctors observe a rash around the left or right side of the body they detect the same as shingles. In case the diagnosis of shingles is unclear, then they usually prescribe lab tests, such as the herpes tests, on cells taken from a blister.
Clinical diagnosis of shingles
Shingles diagnosis is generally done depending on the history of pain experienced on one side of the body, along with the rash and blisters.
Once the rash has appeared the signs and symptoms of shingles (herpes zoster) are often clear enough to make an accurate clinical diagnosis. Diagnosis might be a problem in the absence of a rash (such as in the case of zoster without rash).
In addition to that, doctors may also perform a tissue scraping or culture of the blisters for examination in the laboratory.
Shingles diagnosis in children, younger adults, and people is often difficult. These individuals are more prone to develop atypical presentations due to compromised immune systems. Sometimes herpes zoster is confused with herpes simplex and rarely with impetigo, contact dermatitis, folliculitis, scabies, insect bites, papular urticaria and drug eruptions.
Laboratory methods for shingles diagnosis
Laboratory testing may be of more importance in cases with less typical clinical presentations, as seen in people with suppressed immune systems who may have disseminated herpes zoster.
These include the following:
Polymerase chain reaction (PCR)
The method can be used to detect Varicella zoster virus (VZV) DNA fast and sensitively in carefully collected skin lesion specimens. The availability of PCR testing for VZV is though limited in all settings.
PCR can be used to distinguish between wild-type and vaccine strains of VZV.
Direct fluorescent antibody staining of the varicella zoster virus (VZV)
In this method, the scraping of infected cells from the base of a lesion is rapid, specific and sensitive, however it is relatively less sensitive than polymerase chain reaction (PCR).
This method can also be included on biopsy material and on eosinophilic nuclear inclusions.
Serologic methods
These methods can also be used for laboratory diagnosis of shingles, even though the interpretation of the results are challenging.
Patients with the virus can mount an IgM response but a positive IgM ELISA result could be the result of a primary VZV infection, re-infection or even re-activation.
It is also not easy to identify an increase in IgG for laboratory diagnosis of shingles, since patients may have increased antibody titre from earlier varicella disease.
Tzanck smears
Smear of lesion specimens are inexpensive and can be easily conducted at bedside, although they do not distinguish between VZV and herpes simplex virus infections.
Even after VZV infection is diagnosed by various laboratory methods, it may be difficult to distinguish between varicella and disseminated herpes zoster by physical examination or serological testing, in people with compromised immune systems.
In such situations a history of VZV exposure or of a rash that began with a dermatomal pattern, along with results of VZV antibody testing at or before the time of rash onset can aid the diagnosis protocol.
Can shingles be diagnosed without a rash?
Shingles without a rash is usually unseen. Based on the symptoms alone it is very difficult to detect this disease without a rash.
Doctors may perform various tests such as cerebrospinal fluid tests or saliva tests or blood tests to detect whether VZV antibodies are present. Your doctor can confirm a diagnosis of shingles without a rash through these tests. But, these tests are often inconclusive and do not guarantee that your shingles would be diagnosed.