Treatment of Achalasia
- Updated on: Jul 12, 2024
- 3 min Read
- Published on Feb 6, 2019
Need to treat esophageal achalasia
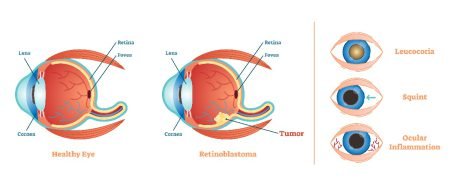
Achalasia is supposed to be a disease of the nerves around the esophagus. It leads to severe complications such as esophageal carcinoma, gastroesophageal reflux disease (GERD), etc. If achalasia is not timely treated, it may result in enlarged esophagus which eventually leads to its abnormal functioning causing such as a difficulty in swallowing. Achalasia results from continuous degeneration of ganglion cells (in the myenteric plexus) in the esophageal wall.
Treatment of achalasia
The main aim during the treatment of achalasia is to reduce the pressure at the lower esophageal sphinter (LES). There is no specific therapy or cure to completely fix it but the symptoms of achalasia can be managed with appropriate treatment.
Patients are treated on the basis of the types of achalasia they suffer with as different types of the disease may need different treatment. According to a research publication titled, “An Overview of Achalasia and Its Subtypes”, achalasia is categorized into 3 distinct types based on manometric patterns. Type 1 (classic) achalasia is classified with minimal contractility in the esophageal body. Type 2 achalasia is classified with intermittent periods of panesophageal pressurization and achalasia type 3 (spastic) is classified with premature or spastic distal esophageal contractions.
It was found that patients with achalasia type 1 react well to both pneumatic dilation and laparoscopic Heller myotomy methods of treatment. Patients with achalasia type 2 show best results with laparoscopic Heller myotomy while type 3 achalasia patients are best treated with pneumatic dilation or POEM (Per-Oral endoscopic myotomy).
Here are listed different types of treatments that are generally used for treating patients with achalasia:
Laparoscopic Heller myotomy
Myotomy is a surgical procedure to weaken LES by cutting the muscle fibers. A laproscopic Heller myotomy procedure is usually recommended by doctors as it improves dysplagia. During the procedure, tiny incisions are made in the abdomen by applying cuts to the muscles at the end of the esophagus and at the top of the stomach to loosen the muscles (lower esophageal sphincter). Dor fundoplication is performed during Heller myotomy which means partially wrapping the upper part of the stomach around the lower part of the esophagus. A small camera is passed into the abdomen through these small abdominal incisions to analyze the condition. This is a minimally invasive procedure that opens the tight lower esophageal sphincter and helps to separate the stomach and esophagus from the surrounding tissues.
Heller myotomy can also be referred to as esophagomyotomy and can be done through the chest. It is observed that more than 80 percent of the symptoms are relieved with this procedure. There are some chances that reflux might occur.
Per-Oral endoscopic myotomy (POEM)
POEM is an endoscopic technique during which a flexible tube with electrical scalpel is passed down to make a cut between the lining of the esophagus and the muscle layer. The scalpel, attached to the endoscope, creates a tunnel within the wall of the esophagus. POEM results are better when compared to those of pneumatic dilation and surgical myotomy. POEM is generally preferred for type 3 achalasia patients.
Per-oral endoscopic myotomy is an emerging endoscopic technique and is also recommended in patients with spastic esophageal disorders when other medical therapies do not give positive results. In some cases, gastroesophageal reflux disease (GERD) is one of its potential side effects.
Other non-surgical methods for achalasia treatment
Pharmaceutical or medical therapy is recommended for patients who are unable or are unwilling to undergo any surgical treatment. Calcium channel blockers or beta blockers are recommended for a medical therapy but these do not work in long-run treatments. Pharmaceutical methods of treating achalasia include such as:
Botox injection treatment
Botulinum toxin injections or Botox injections provide relief for a short period. These injections paralyze the nerves,temporarily that signal the lower esophageal sphinter to contract and help in relieving the obstruction. Botulinum toxin injections are also used occasionally as a diagnostic test for achalasia. About 60 percent of patients are known to benefit from this treatment.
Pharmaceutical treatment is also recommended to extend the time between two dilations. It is studied that these endoscopic injections of toxin are remarkably safe. In a study named “Botulinum toxin for achalasia: long-term outcome and predictors of response” by Pasricha et al, it was reported that a botox injection therapy provides a 30% efficacy rate after a mean follow-up of more than two years. This study finds that Botox therapy can work as a long-term treatment procedure.
Pneumatic dilatation procedure
Pneumatic dilatation is also known as balloon dilation method. Balloon dilation is a traditional non-surgical endoscopic treatment for achalasia. Pneumatic balloon dilatation is considered a highly efficacious procedure. It is estimated that more than 65% of patients will gain positive results after dilatation. The disadvantage of this method is that dilatation needs to be repeated. About 1-2% people also suffer from severe complications during the procedure in case of rupturing of the esophagus.
This technique involves an endoscopy guided procedure. A catheter with a deflated balloon is passed through the mouth and into the stomach. The balloon at the lower esophageal sphincter is inflated for a few seconds with air to create a passage. Some related complications, which occur rarely, are bleeding, perforation in the lining of the esophagus, etc.