Browsing: Myocardial Infarction
Comprehensive Information, Resources, and Support on Myocardial Infarction (Heart Attack)
As we age, our heart’s efficiency can gradually decline, influenced by both the natural aging process and our lifestyle choices.…
How Do You Prevent a Heart Attack Quickly? Which Exercise Is Best for the Heart?
Introduction Heart disease remains one of the leading causes of death worldwide, and preventing a heart attack is crucial for…
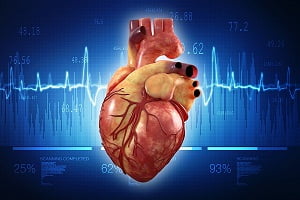
Human Heart: Anatomy, Function, Chambers, Location, Facts
The heart is a muscular organ that works as your body’s circulatory pump. It takes in deoxygenated blood through the veins and delivers it to the lungs for oxygenation and then pumps this oxygenated blood into the arteries. In coronary heart disease, the heart does not function properly. Learn more about your heart.
Sharp Pain in Chest: What It Means and When Should You See a Doctor?
Sharp pain in chest can be caused by anything from usual muscle pain to a severe heart disease. Enlarged or dilated heart can develop as a result of many heart diseases. Some of them can show signs such as pain in chest and breathlessness.
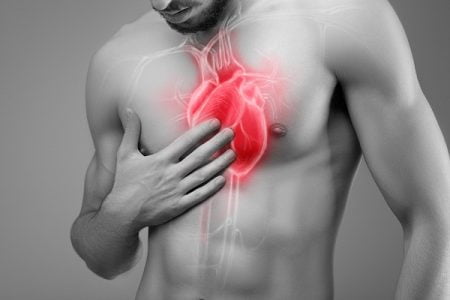
Heart Attack Symptoms in Men
Common signs and symptoms of heart attack in men Symptoms of heart attack (myocardial infarction) can vary from one individual…
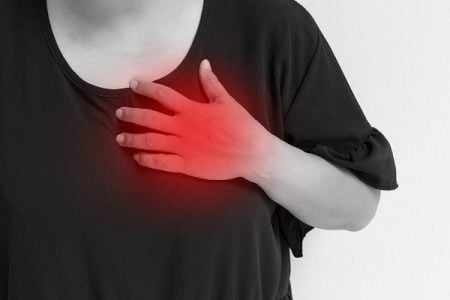
Heart Attack Symptoms in Women
Recently, scientists have found that heart attack symptoms can be quite different for women than for men. The most important…
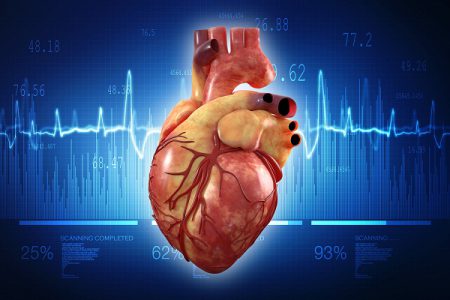
Our Heart during a Heart Attack
Our heart muscle is surrounded by a group of blood vessels, called coronary arteries. The main function of these arteries is to supply oxygen-rich blood and other nutrients. The heart muscle needs an abundant supply of the blood. A heart attack occurs when a coronary artery becomes blocked reducing this blood supply.
Myocardial infarction is commonly known as ‘heart attack’. It is the most common heart condition experienced by people across the world. A myocardial infarction is a life threatening heart condition in which heart muscles experience sudden cut in oxygenated blood supply that results in the damage of heart tissues.
Blood Pressure (BP) During a Heart Attack and Blood Pressure Before a Heart Attack
Blood pressure is the amount of force your blood provides when it is pushed from the heart and circulated to different organs throughout the body. Many people have a doubt about the blood pressure during a heart attack and frequently they ask this question “is blood pressure high during a heart attack”?