How is Prostatitis Diagnosed?
- Updated on: Jul 13, 2024
- 6 min Read
- Published on Oct 3, 2019
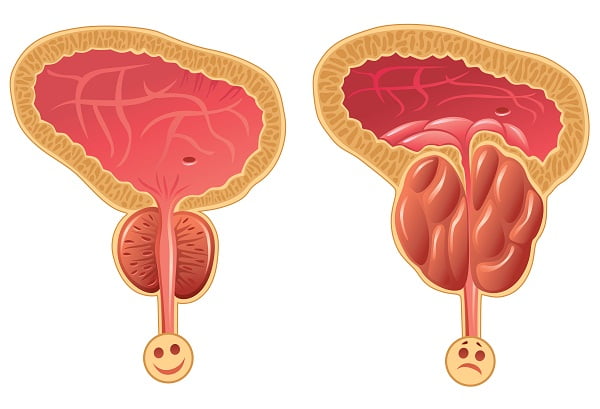
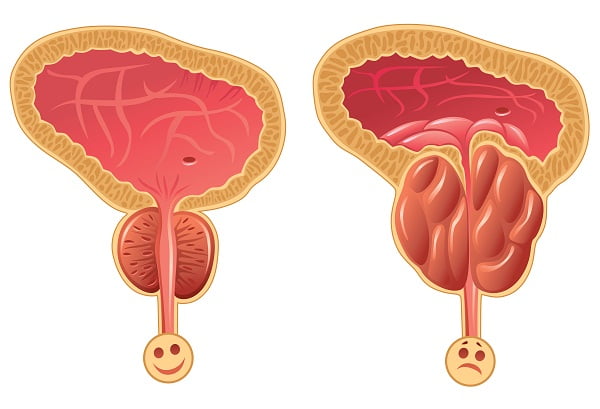
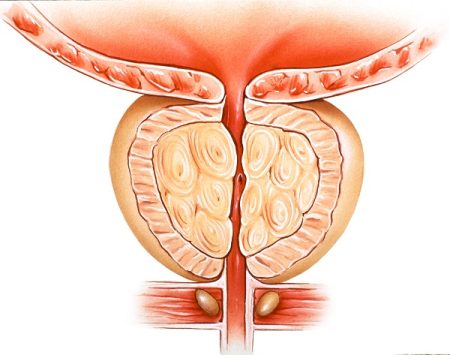
Diagnosis of prostatitis
Diagnosing prostatitis can be quite challenging because of similar symptoms and various causes of prostatitis.
According to a survey, only 5% to 10% of cases are caused by bacterial infection in the prostate gland. Remaining 90-95% cases are Chronic Pelvic Pain Syndrome or CPPS where no bacteria are found.
The causes range from inflammation, stress, autoimmune diseases to genetic and hereditary. Different causes mean different techniques for diagnosis and different treatment options. Doctors may use multimodal approaches to treat the disease.
There are some general tests for prostatitis that doctor performs for its diagnosis. A healthcare professional may begin with medical history and include questions on Chronic Prostatitis Symptoms Index (CPSI) (a test that looks at the scale of the symptoms). However, the type and causes of prostatitis cannot be based solely on the medical history of the patient. The location, severity of pain and other symptoms help in the efficient diagnosis of prostatitis.
Details on urinary tract infection and sexual health may be sought from the patient. For improving the situation and effective treatment, the patient is advised to talk openly with the healthcare professional.
In addition to a thorough analysis of the medical history of the patient, the doctor may also perform a physical examination of the area. This includes an examination of external part of genitalia, scrotum and perineum. Prostate and abdomen are also checked for any sign of inflammation.
The doctor performs a series of tests which are listed below:
- Medical history and symptoms test
- Rectal examination
- Prostate Specific Antigen (PSA) test
- Urine test
- UPOINT test
- Urine Flow Studies
- Four-glass and two-glass test
- Imaging methods
- Cystoscopy
- Milking of prostate
- Other diagnostic tests like blood test
Medical history and symptoms test
This is the very first step for the diagnosis of prostatitis. The doctor or healthcare professional inquires about the symptoms and past medical history of the patient. The patient should share information regarding any urological surgery or trauma experienced.
It is advised to share both family’s as well as personal medical history with the doctor for a better diagnosis. Doctors also perform a basic test called as Chronic Prostatitis Symptoms Index (CPSI). The test also involves asking questions about severity and location of the pain.
Questions associated with the problems in urination and sexual health are included. The answers given by patient will help the doctor monitor the severe symptoms and diagnose the condition.
Rectal Examination
Digital examination of the rectal region is a part of prostate cancer diagnosis as well as prostatitis. As the procedure causes discomfort and pain, the patient doesn’t always go for this option. Relaxing and urinating before the examination sometimes helps the patient to get over the unwanted anxiety.
The procedure is not time taking. With digital rectal examination, doctors determine the size of the prostate and look for any abnormalities in the rectal region. In addition to analyzing the prostate, the doctor also checks the wall of the colon for any anomaly.
Your doctor may ask to bend forward at the waist or may ask to lie on the sides with knees pulled up to the chest. As the patient is in position, the doctor inserts a gloved finger (lubricated) into the rectum and look for the size of prostate and its enlargement.
The patient may feel immediate urge to urinate and slight discomfort. If the prostate is infected or inflamed, the person may feel significant pain during the examination. The doctor sometimes digitally examines the muscles on the side of the prostate to locate the source of pain.
The digital rectal examination is safe and has no side effects.
Prostate-Specific Antigen (PSA) Test
Prostate-specific antigen test is generally used for the diagnosis of prostate cancer but proved helpful in diagnosing prostatitis. As it is a blood test, it needs to be done before digital examination of the rectal area.
The doctor may ask the patient to avoid sexual activity, bike riding and other activities that can cause trauma to the prostate as this may increase the readings of PSA test.
Urine test
Evaluation of urine is also done for diagnosing prostatitis. This is a simple and somewhat common test, also done for the detection of other urinary tract related problems.
For the diagnosis of prostatitis, doctors look for bacteria, white blood cells and proteins in urine samples. It also helps in ruling out the probable cause of prostatitis along with the diagnosis. The urine sample is examined for:
- Turbidity of urine
- Clear nature of urine
- Content
- Concentration
The urine sample may look cloudy if the person is suffering from urinary tract infection. Presence of bacteria in the urine sample confirms prostatitis.
The protein level indicates signs of kidney disease. The doctor can ask the patient to bring urine in a collection cup or can ask for it during the clinic visit. Patients are advised to wash hands before and after urine collection.
Often doctors provide medicated towels to clean the genital area including the penis. Medications and food supplements can affect the test, thus doctors ask for medical history before any test.
UPOINT test
UPOINT is an effective and modern method for the detection of Chronic Pelvic Pain Syndrome (CPPS). It is based on following domains:
- Urinary (U)
- Psychosocial (P)
- Organ-specific (O)
- Infection (I)
- Neurologic/systemic (N)
- Tenderness (T)
The patient is classified as “yes” or “no” for each above-mentioned domains. Once the doctor detects the problem area, the patient can be treated efficiently.
Urine Flow Studies
To see the functioning of lower urinary tract and diagnose prostatitis, doctors may perform urine flow studies. This is also called as Uroflowmetry or urodynamics. It is a quick and non-invasive method.
It determines how fast urine is released as well as the amount of urine released by the person. Any obstruction in the urine flow is verified by this method. The patient is asked to drink four glasses of water and then urinate on a device to record the information.
Four-Glass Test and Two-Glass test
The Meares-Stanley test or Four Glass Test is less often used to diagnose prostatitis. The test takes time and is expensive as compared to other diagnostic techniques.
A shorter version i.e. three-glass test is sometimes used as an alternative to it. This test allows the doctor to look for bacteria and white blood cells (WBCs) in the urine and secretions from the prostate.
For this test, first released urine, midstream urine, secretions from prostate after prostate massage and urine after the prostate massage is taken.
Pre- and Post-massage test or PPMT is a simple and less time-consuming test for the detection of prostatitis. It is sometimes also called as “two-glass” test. The doctor collects the urine sample before as well as after prostate massage for the analysis of any signs of bacterial infection. The results from this test are said to be 90% accurate.
Imaging methods
For a clear diagnosis of prostatitis, the doctor may sometimes opt for MRI, ultrasound and other imaging tests. These tests are often done when the doctor suspects bacterial infection to be the reason for prostatitis.
In severe cases, the infection may spread beyond the prostate. If the doctor suspects that the patient may have kidney issues or prostate cancer, he/she may ask for imaging tests for drawing a clear conclusion.
Cystoscopy
Cystoscopy is not used for every patient. The healthcare professional inserts a cystoscope into the penis to get a view of the bladder and urethra. Doctors get an idea how hard the prostate squeezes the bladder and check for any residual urine after urination.
With this procedure, doctors rule out any possibility of prostate stones and presence of diverticula in the prostate. The procedure can be extremely painful and is performed with local, spinal or general anesthesia.
Often the patient feels hard to urinate and swelling in urethra after this test.
Milking of prostate gland
Milking of the prostate gland or commonly called, as prostate massage is a technique to improve blood flow in the prostate gland.
The technique helps to deliver more nutrients and oxygen to the prostate. This eliminates the toxins from the gland and help in the diagnosis of prostatitis. To massage the prostate, the doctor asks the patient to bend forward on a table and relax. The doctor then inserts a lubricated gloved finger into the anus and applies a gentle pressure to massage the prostate.
If done correctly, the procedure does not cause any pain.
Other Diagnostic tests
In addition to the above-mentioned tests, your doctor may perform other tests for the diagnosis. The doctor may perform blood test if the symptoms suggest fever and chills due to bacterial prostatitis.
Along with MRI and ultrasound, computed tomography (CT) scan is also advised to help in verifying spread of the infection. Men who have a history of recurring urinary tract infection are often suggested imaging procedures. Kidney issues and prostate stones are ruled out with the help of these procedures.
More tests may be needed in the cases where:
- there is abscission in bladder and prostate
- there is no improvement in the symptoms after treatment
- there is a continuation in prostate infection
- there are chances of prostate cancer and bladder cancer
FAQs
Can prostatitis be diagnosed without a physical examination?
No, a physical examination is crucial for prostatitis diagnosis. Along with medical history, the doctor may perform a digital rectal exam (DRE) to assess the prostate's condition.
Are there specific tests for diagnosing prostatitis?
Yes, various tests like urine analysis, blood tests, and imaging studies are used. The doctor may also order a prostate-specific antigen (PSA) test to rule out prostate cancer.
How long does it take to get prostatitis test results?
The duration varies, but results from urine and blood tests may be available within a few days. However, some tests, like cultures, may take longer, depending on the laboratory.
Is a biopsy necessary for prostatitis diagnosis?
Generally, no. Prostatitis is diagnosed through less invasive methods. Biopsies are more common in suspected prostate cancer cases.
Can prostatitis be diagnosed without experiencing symptoms?
It's challenging. Symptoms are crucial for diagnosis, but in some cases, asymptomatic individuals may be diagnosed through routine screening or during unrelated medical exams.